David S Ettinger, M.D.
- Alex Grass Professor in Oncology
- Professor of Oncology

https://www.hopkinsmedicine.org/profiles/results/directory/profile/0009782/david-ettinger
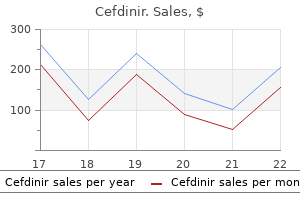
How does one determine whether swallowed maternal blood is the cause for gastrointestinal bleeding in the neonate? For this test 1 part stool is mixed with 5 parts water and centrifuged for 2 minutes to separate out fecal material antimicrobial therapy definition generic 300mg cefdinir overnight delivery. After 2 minutes there is a color change; if the hemoglobin is fetal antibiotic resistant superbugs generic cefdinir 300mg free shipping, the color stays pink; if it is from the mother antibiotic used for acne buy cefdinir 300 mg without a prescription, it turns yellow-brown antibiotic kanamycin discount 300mg cefdinir fast delivery. What is the first step in the management of an acutely ill infant with significant gastrointestinal bleeding? The key initial step is to obtain stable intravenous access for patient resuscitation. Particularly with hematemesis, the rapidity and severity of gastrointestinal bleeding can be significant, and the need for urgent intravenous access should not be underestimated. Breast milk offers many nutritive advantages in addition to protective immunologic substances. Milk macrophages and phagocytes, immunoglobulins A and G, and immunocompetent T and B lymphocytes may offer a protective advantage to the mucosa. These components potentiate the effect of the complement components C3 and C4, lysozyme, lactoferrin, and secretory immunoglobulin A. Breast milk also favors the growth of Lactobacillus bifidus and promotes the development of a healthy gut microbiome. Large-volume milk feedings that are increased too rapidly during the feeding schedule may place undue stress on a previously injured or immature intestine. Volume increments probably should not be more than 20 to 35 mL/kg/day and should be advanced on the basis of the clinical examination, physiologic stability, and feeding tolerance. Slow advancement of enteral feed volumes to prevent necrotising enterocolitis in very low birth weight infants. However, a higher incidence of sepsis was reported in those infants receiving probiotics. Thus probiotics can be considered but should be used with caution, based on current data. To date, no large-scale trial of probiotics has been successfully carried out, and there are currently many different bacterial components in available probiotics. No probiotic is currently approved by the Food and Drug Administration for neonatal use. Malabsorbed carbohydrates are fermented by colonic bacteria and cause increased intestinal gas production, resulting in abdominal distention. This gas, which is 30% to 40% hydrogen gas, dissects into the submucosa and subserosa, producing pneumatosis intestinalis. High intraluminal pressure resulting from gaseous distention may reduce mucosal blood flow, producing secondary intestinal ischemia. It is important to emphasize that, unlike in adults, Clostridium difficile and associated toxins are found in the intestinal tracts of many neonates who are entirely asymptomatic. The asymptomatic carrier state in some infants may be due to differences in intestinal immaturity, local differences in the intestinal milieu, absence of toxin-related receptors, or other protective factors. The antibiotics were stopped after 3 days because the blood culture results were negative. He began enteral gavage feeds on day 5, at 20-cc/kg/ day increments, and finally achieved "full feeds" (150 cc/kg/day) by day 20. He then developed an increased frequency of apnea and bradycardia associated with temperature instability. Management includes the following: (1) consultation with a pediatric surgeon, (2) withdrawing all enteral feeds, (3) gastric decompression by placing an orogastric tube to low wall suction, and (4) beginning antibiotics after appropriate cultures are collected. One day after beginning appropriate management, the same infant (see Question 151) develops persistent abdominal distention, right lower quadrant tenderness, and diminished bowel sounds. These clinical findings may herald the beginning of dilated viscus, submucosal or subserosal dissection of air, and peritonitis.
Hypercarbia cowan 1999 antimicrobial generic cefdinir 300mg line, hemodynamic impairment virus alive cefdinir 300 mg otc, and air leak caused by incomplete exhalation occur when the expiratory time is too short to allow complete exhalation before the next mechanical breath occurs antimicrobial drugs discount cefdinir 300mg on-line. This situation is most likely to occur in infants who have increased airway resistance antibiotic resistance pbs generic 300mg cefdinir visa, such as is seen in meconium aspiration with acute airway obstruction or in chronic lung disease in which airway edema, copious secretions, and bronchospasm are present. What is a time constant, and why is it important to consider when ventilating a newborn infant? A time constant is the product of lung compliance and airway resistance (Tc = R Ч C). Conceptually, time constants reflect the time it takes for gas flow to cease and pressure to be fully equilibrated between the large airways and the alveoli when a sudden pressure change is applied to the airway opening (three time constants are needed for 95% equilibration). In addition, time constants are also a function of size (total compliance, not compliance per kilogram, is used). Consequently, large subjects such as adults or horses have long time constants, and small premature infants and hummingbirds have short time constants. Time constants are a major determinant of resting respiratory rate, which turns out to fall exactly where work of breathing is lowest. This is why adults at rest breathe at a rate of 14 breaths per minute, term infants breathe at 40 breaths per minute, and small premature infants breathe at about 60 breaths per minute. In infants with acute respiratory distress, tachypnea is a reflection of shorter time constants as lung compliance decreases because of various causes. Asthmatics, on the other hand, prefer to breathe rather slowly because of their prolonged expiratory phase. The bottom line is this: Consider the underlying disease process and its pathophysiology before making decisions about ventilator settings. A percentage change in pressure in relation to the time (in time constants) allowed for equilibration. As a longer time is allowed for equilibration, a higher percentage change in pressure occurs. Optimize oxygen delivery and prevent hyperoxia and hypoxia (by carefully adjusting FiO2 levels). A/C ventilation is a form of mechanical ventilation in which the infant triggers the ventilator to cycle with each breath. With a small triggering effort, therefore, the baby can achieve a much higher level of ventilatory support than with spontaneous breathing. It has become the most common way to initiate mechanical ventilation therapy in these clinical situations. With synchronized intermittent mandatory ventilation, the loops are either triggered by the patient or the ventilator. In A/C mode, every breath that the infant takes triggers a ventilator breath-that is, every breath is supported. Why does hand ventilation with a bag often work when mechanical ventilation is failing? In a crisis it is frighteningly easy to inadvertently generate pressures above 40 cm H2O. This approach allows you to continue to use the monitoring function of the ventilator to provide feedback regarding the tidal volume and other parameters, and it provides controlled and accurate pressure delivery. However, if the baby is still doing poorly, hand ventilation is an acceptable alternative. When a baby is doing poorly on a ventilator, the clinician should remove the baby from the machine and hand ventilate with an anesthesia (preferably) or self-inflating bag. A chest radiograph is often helpful to ensure proper positioning of the tube and to confirm that no air leak is present. If the tube seems fine and there are no radiologic changes, the ventilator itself must be carefully checked for malfunction. Respiratory therapists should be available around the clock in any intensive care nursery in which infants are ventilated. Although there is a great deal of literature on neonatal intubation, few articles describe the risks of extubation. Nothing is more frustrating than successfully completing a course of neonatal mechanical ventilation on a sick baby only to have a serious setback because of a poor effort at extubation. When a child has reached the predetermined levels for extubation, the following should be done: n A chest radiograph should be obtained as a baseline so that postextubation changes can be compared. However, these adjuncts may be useful if one or two prior attempts at extubation have failed.
Valproic acid may cause neural tube defects antibiotic resistance what can be done purchase 300mg cefdinir with amex, and diphenylhydantoin is associated with fetal hydantoin syndrome antibiotic dosage quality cefdinir 300mg. The effects of other psychotropic agents on the fetus appear minimal antibiotic resistance threats cdc generic 300mg cefdinir with visa, but some cases of teratogenesis have been reported antibiotic resistance quiz trusted cefdinir 300mg, especially with some benzodiazepines. The critical issue that remains unresolved, however, is whether these drugs alter the development of the maturing fetal central nervous system. Maternal Graves disease can result in neonatal thyroid storm and hyperthyroidism in rare cases. It is associated with a high risk of both structural abnormalities and mental retardation in the newborn. Both can cause malformations of the skull and bones as well as mental retardation. Prednisone and prednisolone cross the placenta to a small degree and therefore are the drugs of choice during gestation. Sulfa drugs may accentuate hyperbilirubinemia during the neonatal period by displacing bilirubin from binding sites. Sulfamethoxazole/trimethoprim has been associated with congenital cardiac defects. Most other antibiotics (including acyclovir) appear to be safe for use during pregnancy. Indomethacin has been used frequently as a tocolytic agent and is also reported to produce ductal closure, but it appears to be reasonably safe with careful fetal monitoring. These drugs do not appear to be teratogens; however, platelet aggregation is also reduced by many of these agents and may increase the potential for bleeding. Symptoms include mental retardation, craniofacial abnormalities, and growth failure. Withdrawal typically begins in the immediate newborn period and lasts for days to weeks. With some narcotics, such as methadone, withdrawal may not be seen for several days. Babies of mothers who use narcotics appear to have an increased risk of abortion, prematurity, and growth failure. Birth weight is generally slightly lower than normal, and there is an increased risk of prematurity. Organ infarction may lead to bowel atresia, porencephaly, and limb maldevelopment. Obstetricians must balance this risk against the serious maternal and fetal risks of untreated depression. Although this list is relatively complete for many of the drugs known to produce significant fetal problems, the practitioner should always review the most recent medical literature for any updates that might reflect changes in awareness of potential risks of drugs during pregnancy. The same is true of breast milk; most medications enter maternal milk to some degree. Few drugs, however, appear in sufficient concentration to have an adverse effect on the fetus or neonate. Patient- and family-centered care is an approach to planning, delivery, and evaluation of health care that supports partnerships among patients, families, and health care practitioners. It is founded on the principle that the family plays a vital role in ensuring the health and well-being of the infant. Family-centered care provides care to families in a manner that involves respect and empowerment and responds to individual diversity and strengths. Changing the concept of families as visitors: supporting family presence and participation. According to the American Hospital Association and Institute for Family Centered Care 2005, the principles are as follows: (Table 4-1) 3. Dignity and respect Health care practitioners listen to and honor patient and family perspectives and choices. Patient and family knowledge, values, beliefs, and cultural backgrounds are included in the planning and delivery of health care.
Cefdinir 300mg generic. Medical Edge: Superbugs.
References
- Pepi M, Muratori M. Echocardiography in the diagnosis and management of pericardial disease. J Cardiovasc Med (Hagerstown). 2006;7(7):533-544.
- Xu J, He L, Ahmed SH, et al. Oxygen-glucose deprivation induces inducible nitric oxide synthase and nitrotyrosine expression in cerebral endothelial cells. Stroke 2000;31(7):1744-51.
- Aldonyte R, Jansson L, Piitulainen E, et al. Circulating monocytes from healthy individuals and COPD patients. Respir Res 2003; 4: 11.
- Chambless LE, Shahar E, Sharrett AR, et al. Association of transient ischemic attack/stroke symptoms assessed by standardized questionnaire and algorithm with cerebrovascular risk factors and carotid artery wall thickness. The ARIC study, 1987-1989.
- Young DS: Conveying the importance of the preanalytical phase. Clin Chem Lab Med 41:884-887, 2003.
- Djajadiningrat RS, Jordanova ES, Kroon BK, et al: Human papillomavirus prevalence in invasive penile cancer and association with clinical outcome, J Urol 193:526n531, 2015.
- White JJ, Neuwirth H, Miller CD, et al: DNA alterations in prostatic adenocarcinoma and benign prostatic hyperplasia: detection by DNA fingerprint analyses, Mutat Res 237(1):37n43, 1990.















